Skin Ulcerations Secondary to Monkeypox (Mpox): Clinical Considerations for Wound Care in Africa
Introduction
Mpox (formerly known as monkeypox) is a zoonotic viral infection caused by the Monkeypox virus, an orthopoxvirus related to the Variola virus. Although historically considered a rare infection outside endemic regions, mpox has gained global attention due to outbreaks in recent years, including the widespread international outbreak in 2022.
One of the hallmark clinical features of mpox is its characteristic skin lesions. These lesions typically evolve through several stages—macules, papules, vesicles, pustules, and finally crusts. In some cases, particularly when lesions are extensive, secondarily infected, or located in areas subject to pressure or friction, they may progress to ulceration.
For clinicians involved in wound care, especially in African settings where mpox is endemic, managing these ulcerations is an important aspect of patient care. Proper wound management can reduce pain, prevent secondary infection, and minimize long-term complications such as scarring.
Epidemiology in Africa
Mpox is endemic in several parts of Central and West Africa. The disease was first identified in humans in the Democratic Republic of the Congo in 1970. Since then, the majority of reported cases have occurred in countries including Nigeria, the Central African Republic, Cameroon, and the Republic of the Congo.
Transmission typically occurs through:
-
Direct contact with infected animals (often rodents or small mammals)
-
Human-to-human transmission through skin lesions, respiratory droplets, or contaminated materials
-
Sexual transmission
Two major viral clades have historically been described: the West African clade and the Congo Basin clade. The latter has generally been associated with higher severity and mortality.
Several factors contribute to the ongoing presence of mpox in Africa:
-
Close interaction between humans and wildlife
-
Limited access to healthcare in rural areas
-
Reduced population immunity since the discontinuation of routine smallpox vaccination
Recent surveillance suggests that mpox may be underdiagnosed in many regions due to limited laboratory capacity and overlapping clinical features with other rash illnesses, such as varicella.
General Treatment of Mpox
Most cases of mpox are self-limiting and resolve within 2–4 weeks. Management is therefore largely supportive, focusing on symptom relief and prevention of complications.
General supportive measures include:
-
Adequate hydration and nutrition
-
Antipyretics and analgesics for fever and pain
-
Isolation measures to prevent transmission
-
Monitoring for complications such as secondary bacterial infection
In severe cases or among high-risk patients, antiviral therapy may be considered. One antiviral that has been used in certain settings is Tecovirimat, which inhibits viral replication and has shown activity against orthopoxviruses. Access to such treatments in many African settings remains limited, however.
Other important aspects of care include treatment of bacterial superinfection and management of complications involving the eyes, respiratory tract, or skin.
Management of Skin Ulcerations
While many mpox lesions heal without intervention, some lesions—especially larger pustules or those complicated by bacterial infection—may progress to ulceration. These ulcers may be painful, slow to heal, and susceptible to secondary infection.
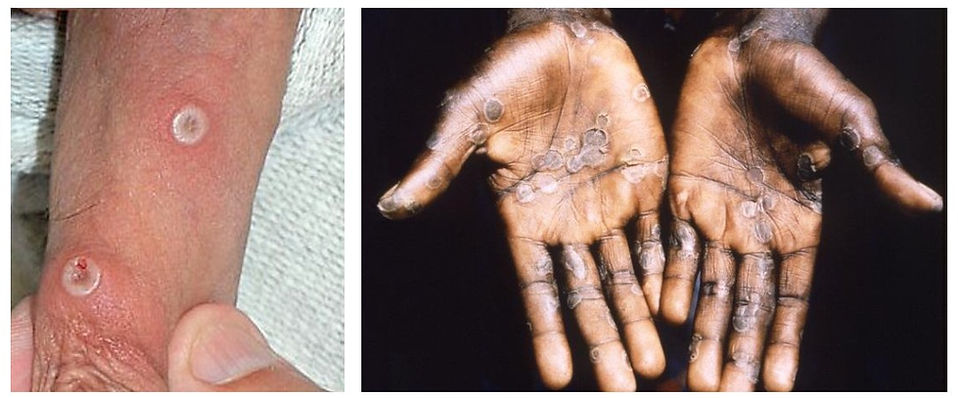
Images 1 & 2:
Left image: Mpox lesions on a penis. This illustrates the characteristic ring-like lesion, typically accompanied by inflammation in the surrounding skin. In this inflammatory phase the lesions can be quite painful, particularly in the genital or perineal area.
Right image: Multiple lesions that have started to dry out and are in the healing phase.
Copyright left image: Dr. Graham Beards; licensed under the Creative Commons Attribution-Share Alike 4.0 International license.
Copyright right image:Brian W.J. Mahy; (CDC's Public Health Image Library) Media ID #12761

Image 3: Progression of necrotic mpox lesion after needlestick injury from a pustule. At the stage in image B, the lesion is usually quite painful due to the inflammation. Note that an ulcer developed although there was no obvious signs of a secondary infection.
Copyright: João P. Caldas, Sofia R. Valdoleiros, Sandra Rebelo, and Margarida Tavares - https://wwwnc.cdc.gov/eid/article/28/12/22-1374-f1
Should Mpox Lesions Be Opened?
In general, mpox lesions should not be intentionally opened or de-roofed. The vesicles and pustules that characterize Mpox contain high concentrations of viral particles, and opening them unnecessarily may increase the risk of viral transmission, secondary bacterial infection, and delayed healing.
Most mpox lesions follow a predictable natural evolution—from macule to papule, vesicle, pustule, and finally crust—after which they gradually re-epithelialize. When left undisturbed, this process usually results in uncomplicated healing over a few weeks.
However, we have seen that some lesions heal much faster when they are de-roofed and treated with an antimicrobial tincture, such as 2% Gentian violet, 10% povidone iodine, or soaked in potassium manganate. It is our opinion that especially when there is a lot of inflammation around a solitary lesion and it is particularly painful, deroofing it and drying it out with desiccating tinctures may be a good solution. If you have opened a lesion, it should be covered with an absorbent material to limit transmission of the virus. We recommend gauze soaked in povidone iodine to cover the lesions. This aids in drying out the lesions and may prevent secondary infection. We treat spontaneously ruptured lesions in the same manner. Consider applying Gentian violet daily and changing the iodine dressing every day as well. Both Gentian violet and 10% Povidone iodine are usually available even in remote areas with low resources.
If you are a healthcare provider working in an area of Africa where you more frequently treat mpox lesions, our readers would appreciate any other advice you can provide. Please contact us via email. If you do a search on google/other search engines or do a query using AI, you will discover that there is not so much available about this topic.

Image 4: Gentian violet (preferably at 2% concentration), Povidone Iodine (10%), and Potassium permanganate all have adstringent, desiccating, and antimicrobial properties and can be used to dry out a mpox lesion. For isolated lesions, our first choice would be to paint the lesion daily with 2% gentian violet and cover it with iodine gauze. If the patient has numerous lesions on an extremity, for example, potassium permanganate soaks or compresses are more practical. Potassium permanganate should be diluted to around 0.01% for soaks up to 20 minutes. The solution should appear light pink, not dark purple, to avoid chemical irritation or burns. Soak the lesions/ cover with soaked compresses for 20 minutes. You do not need to rinse it off. Note that all the substances can permanently stain clothing and furniture, so precautions should be taken when using them.
Image 5: The WHO has published a practical guide for treating mpox lesions. This can be downloaded by clicking on the image above. Copyright: World Health Organization
Practical Wound Care Tips for Mpox Lesions in Low-Resource Settings
Clinicians managing skin lesions caused by Mpox often work in settings where access to advanced wound care products is limited. Fortunately, many lesions can be managed effectively using simple principles of hygiene, protection, and infection prevention.
1. Do not routinely open lesions
Mpox vesicles and pustules contain large amounts of the Monkeypox virus. Lesions should generally be left intact, as the roof acts as a natural biological dressing. Opening lesions increases the risk of viral transmission and secondary bacterial infection. If lesions rupture spontaneously, the wound should be gently cleaned and protected.
2. Keep lesions clean
Daily gentle cleansing with clean water or saline is usually sufficient. Where available, mild antiseptics may be used if there are signs of bacterial colonization.
3. In selected cases, especially isolated lesions with more inflammation and significant pain, de-roofing and desiccation with 2% gentian violet (our primary choice) or 10% povidone iodine can be done. Spontaneously ruptured lesions can be treated the same way. The lesions should be painted daily with these solutions until dry.
4. Consider potassium permanganate for extensive lesions
The World Health Organization suggests that dilute potassium permanganate soaks or compresses may be helpful when lesions are widespread, moist, or difficult to keep clean. Very dilute solutions (approximately 0.01%, appearing light pink) can help dry weeping lesions and reduce bacterial colonization.
4. Protect ulcerated lesions
When lesions rupture or become ulcerated, non-adherent dressings can help protect the wound and reduce pain during dressing changes. In many settings, simple gauze with a layer of petroleum jelly may serve as an effective low-cost alternative.
5. Watch for secondary bacterial infection
Signs such as increasing pain, redness, purulent discharge, swelling, or fever may indicate bacterial infection. In such cases, systemic antibiotics may be required according to local guidelines.
6. Reduce friction and pressure
Lesions in areas such as the genitals, buttocks, or thighs may worsen with friction or pressure. Loose clothing, protective dressings, and minimizing prolonged pressure can help prevent ulceration.
7. For painful lesions in the genital or perineal area, topical analgesic creams or gels may provide some temporary relief.
7. Protect healthcare workers and caregivers
Because an infectious virus is present in lesion fluid and crusts, healthcare workers should use gloves, good hand hygiene, and appropriate protective equipment when managing wounds.
Differential diagnosis of Mpox
In endemic regions, the diagnosis of mpox may be relatively straightforward when patients present with multiple characteristic lesions across multiple body sites, along with systemic symptoms. However, clinicians should remain cautious when lesions are localized, particularly in the genital or perianal area, where mpox may easily be mistaken for sexually transmitted infections such as herpes simplex or syphilis.
When evaluating patients with lesions suspicious for Mpox, it is important to consider several differential diagnoses, particularly because many infectious diseases can present with vesicles, pustules, or ulcerative skin lesions.
Important Differential Diagnoses of Mpox:
Other Orthopoxvirus Infections
-
Smallpox (eradicated but historically similar presentation)
-
Cowpox
-
Vaccinia
These infections may produce pustular lesions similar to those of mpox, though they are rare in most settings today.
Varicella and Other Viral Exanthems
-
Varicella
-
Herpes zoster
Varicella can resemble mpox, particularly early in the disease. However, varicella lesions typically appear in different stages simultaneously and are more superficial.
Herpes Simplex Infection
-
Herpes simplex
Herpes simplex virus infection is an important differential diagnosis, particularly for genital or perianal lesions. HSV lesions usually present as painful grouped vesicles that rupture into shallow ulcers, often recurring in the same location.
Sexually Transmitted Ulcerative Diseases
Lesions in the genital or perianal area may easily be confused with STIs such as:
-
Syphilis (primary chancre)
-
Chancroid
-
Lymphogranuloma venereum
These conditions may produce genital ulcers and lymphadenopathy, which can overlap with the clinical presentation of mpox.
Bacterial Skin Infections
-
Impetigo
-
Ecthyma
These infections may produce crusted or ulcerative lesions, especially in children.
Parasitic and Tropical Ulcerative Diseases
In parts of Africa, clinicians should also consider:
-
Cutaneous leishmaniasis
-
Yaws
-
Buruli ulcer
These diseases can cause chronic ulcerative skin lesions, though they usually evolve more slowly than mpox.
Features that may help distinguish mpox include:
-
Deep-seated, firm lesions
-
Lesions often progress synchronously through stages
-
Prominent lymphadenopathy
-
Associated with fever and systemic symptoms
-
Lesions appearing on the face, extremities, and genital areas simultaneously
-
Laboratory confirmation with PCR testing of lesion material remains the gold standard for diagnosis. This is not readily available in many parts of the continent.
References:
World Health Organization.
Clinical management and infection prevention and control for monkeypox: Interim rapid response guidance.
Geneva: WHO; 2022.
https://www.who.int/publications/i/item/WHO-MPX-Clinical-and-IPC-2022.1
World Health Organization.Mpox (monkeypox): Fact sheet.
Geneva: WHO; updated regularly.https://www.who.int/news-room/fact-sheets/detail/mpox
Centers for Disease Control and Prevention.Clinical Recognition and Treatment of Mpox.
CDC; 2023–2024.
https://www.cdc.gov/mpox/hcp/clinical-care/index.html
Anne W. Rimoin, et al. Major increase in human monkeypox incidence 30 years after smallpox vaccination campaigns cease in the Democratic Republic of Congo.
Proceedings of the National Academy of Sciences. 2010;107(37):16262–16267.
Brian W. J. Mahase.
Monkeypox: what do we know about the outbreaks in Europe and North America?
BMJ. 2022;377:o1274.
Daniel Bausch & Anne W. Rimoin.
Monkeypox: Epidemiology, pathogenesis, and clinical features.
Lancet Infectious Diseases. 2022.
Africa Centres for Disease Control and Prevention.
Mpox (Monkeypox) Outbreak Situation Reports and Clinical Guidance.
https://africacdc.org/disease/mpox/
John H. Beigel et al.
Tecovirimat for the treatment of orthopoxvirus infections.
New England Journal of Medicine / Clinical Infectious Diseases discussions of antiviral therapy.
Rook's Textbook of Dermatology.
Latest edition. Wiley-Blackwell.


























