Pyoderma gangrenosum
Pyoderma gangrenosum (PG) is a skin disease that all wound care practitioners should be familiar with, even though it is a relatively rare diagnosis. The condition may become aggressive if the wound is manipulated with debridement or surgical excision of tissue. Therefore, when PG cannot be ruled out, one must be cautious about revising or debriding the wound.
The abbreviation PG can be misleading. Another dermatological condition—pyogenic granuloma—is also abbreviated PG, but it is a completely different condition.
PG wounds are challenging, and treatment should be managed by professionals experienced in this condition. PG is primarily treated by dermatologists. This is not a condition that requires the patient to wait weeks for an assessment by a dermatologist. It is a “semi-urgent” condition that should be evaluated by a dermatologist within a few days.
At the end of this chapter, you will also find a collection of articles and videos about the diagnosis of pyoderma gangrenosum.
What is pyoderma gangrenosum?
PG is a fairly rare, chronic autoimmune inflammatory skin disease. In the Western world, the incidence is approximately 1 per 100,000 inhabitants.
The disease most commonly affects adults aged 20 to 50 and can present in several ways. It can basically mimic any other type of ulceration, and many clinicians often go into a trap initially. This often leads to a delayed diagnosis, which may result in the wounds becoming larger and deeper and therefore more difficult to treat.
In at least half of cases, the condition is associated with rheumatoid arthritis, inflammatory bowel disease (ulcerative colitis or Crohn’s disease), and myeloproliferative disorders (for example, myelogenous leukemia), as well as chronic active hepatitis.
The condition often develops after a minor trauma to the lower leg. It is not uncommon for it to begin as a harmless bruise or small hematoma that later becomes painful, with ulcer formation. In other cases, the wound starts as a small “pimple” or "pustule". Over time, several small ulcers may develop and merge into a larger wound.
If PG is suspected, the patient should be referred to a dermatologist or a dermatology department.

Figure 1. Because pyoderma gangrenosum often mimics other types of chronic ulcers, it is unfortunately common that the diagnosis is significantly delayed. Even experienced clinicians often fail to diagnose the condition initially. From our own experience at our own clinic, we failed to diagnose it correctly at the start in at least half of the cases we see. The image above was created using OpenAI.
What does pyoderma gangrenosum look like?
PG can resemble most types of wounds and is therefore often not diagnosed in its early stages. When PG manifests on the lower extremities—where it most commonly occurs—it is particularly difficult to recognize because it may resemble venous ulcers, arterial ulcers, or diabetic ulcers. Most clinicians who have worked with wound care for a long time have fallen into this trap. If a wound does not behave as expected, PG should be considered.
It may be somewhat easier to suspect PG when ulcers appear in other locations, such as the groin, trunk, or arms, because wounds in these areas are less common and therefore more likely to prompt earlier consideration of differential diagnoses.
In classic PG, one or more ulcerations are seen. They are often well-demarcated but deep. A slightly purple or bluish undermined wound edge is a fairly strong indication that the lesion may be PG. It is typical that a grayish, pus-like fluid can be expressed from the wound bed or from beneath the wound edges. The ulcers are often extremely painful. Pain is an important diagnostic clue. If the wound looks unusual and the patient has more pain than expected, PG should be considered.
The patient may have reduced general condition with fever, joint pain, and muscle pain, although these symptoms are not always present.
Even though we have gained considerable experience in wound treatment over time, we, too, have fallen into this trap several times. Our most important advice is therefore: if a wound does not behave as expected, refer the patient to a dermatologist for further evaluation and diagnosis.

Figure 2. Pyoderma gangrenosum can present in many different ways and may resemble several other types of chronic wounds.
Top left: PG that developed after a minor contusion to the lower leg, initially presenting as a small hematoma. Several small ulcers subsequently appeared and merged into a larger ulcer.
Top right: PG that developed in the scar following hip surgery.
Bottom left: Classic appearance of PG with a violaceous (purple-reddish) wound edge.
Bottom right: Pustular PG that began as small pimple-like lesions before progressing to ulcerations.
Are there different forms of PG?
PG is classified into seven clinical variants:
1. Classic/ulcerative PG
This is the most common form of PG. It progresses rapidly and often begins with a pustule that quickly develops into a painful ulcer. This type of PG is frequently associated with inflammatory bowel disease.
2. Pustular PG
In pustular PG, pustules develop in the skin, typically during periods of increased disease activity in inflammatory bowel disease. The lesions often improve in parallel with treatment of the underlying disease.
3. Bullous/atypical PG
Tender blisters develop, enlarge, and eventually become superficial ulcers with necrosis. This condition is often associated with hematological malignancies.
4. Vegetative PG
This type of PG often lacks undermined wound edges. The lesions are usually single superficial ulcers, often quite large. Pain is less pronounced, and the course tends to be more chronic. The diagnosis of PG is made based on the patient’s medical history and the clinical course.
5. Peristomal PG
Ulcers develop around a stoma or in/around surgical incisions. This type is most commonly seen in patients with inflammatory bowel disease. In many patients with a stoma, PG develops within 3–6 months of stoma creation. Stomas that leak frequently or where the surrounding skin is irritated for other reasons appear to have a higher risk of developing PG.
6. Postoperative PG
When PG occurs in surgical wounds, it most often develops within a few weeks after surgery. In many cases, it appears before the sutures are removed. Many surgeons mistakenly interpret this as wound necrosis or infection and proceed to debride the affected areas. This usually worsens the situation and leads to even larger wounds.
7. Drug-induced PG
This type of PG is being seen increasingly as certain medications are used more frequently. Immunomodulatory drugs, retinoids, and glucagon are particularly known to trigger PG in predisposed individuals. Some recreational drugs (e.g., cocaine) may also trigger PG in susceptible people.
Figure 3. We recommend this article by Witstock and Kanjee, published in 2023 in The Journal of the Wound Healing Society in Southern Africa. The article highlights three illustrative patient cases. Click on the image above to get to the article. Image copyright: WHASA
How is pyoderma gangrenosum diagnosed?
There is no specific test for PG yet. The diagnosis is made based on the clinical appearance and behavior of the wound, together with the patient’s medical history. The most important point is that we, as wound care clinicians, consider this diagnosis when we encounter a wound that behaves differently than expected. When a painful ulcer continues to enlarge despite seemingly adequate treatment, PG should be suspected.
But what about a biopsy—doesn’t that help establish the diagnosis? Unfortunately, diagnosing PG based on histology alone is not straightforward. Pathologists often see infiltration of the dermis by neutrophilic granulocytes, with secondary dermatitis changes, in biopsies from PG lesions, but these findings may also occur in other skin diseases. A biopsy of a suspected PG ulcer is obligatory to exclude other diagnoses, such as a malignant ulcer.
Some pathologists believe they can diagnose PG based on a good biopsy (it is important to take samples from the border between the ulcer and healthy skin), but most pathologists say it is difficult. Histological findings vary depending on the type of PG, the stage of the disease at the time of biopsy, and the exact location within the wound from which the biopsy is obtained.
The best place to take a biopsy is from the red inflammatory zone surrounding the wound edge. Remember to take at least three biopsies. Pathologists generally prefer large biopsy samples, especially for diagnosing PG, and many recommend a 6-mm punch biopsy for this purpose.
Be careful to clearly state in the pathology referral that PG is suspected. Remember that the pathologist has usually not seen the wound, and your clinical information is therefore crucial for interpreting the histological findings!
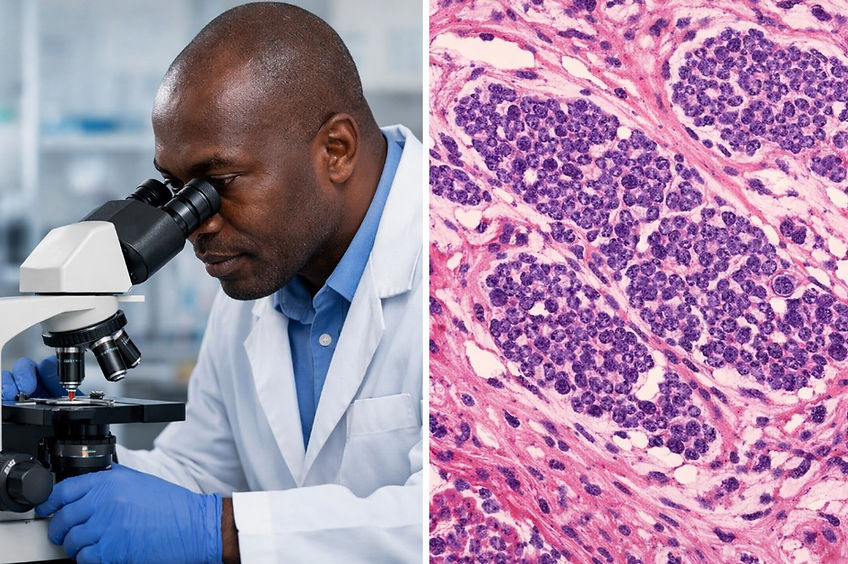
Figure 4. A rule of thumb in wound care is that we should take biopsy of any lesion or ulceration that looks suspicious or does not improve to standard care within 4- 6 weeks. Unfortunately pyoderma gangrenosum presents some challenges to the pathologist as in many cases the condition is hard to spot in a biopsy. To help the pathologist it is important that you specify that you would like them to look for signs of PG and add as much relevant clinical information as possible. Very often you will get a report from the pathologist stating " Findings are nonspecific but may be consistent with PG.”
How is pyoderma gangrenosum treated?
Pyoderma gangrenosum is most often treated systemically with anti-inflammatory or immunosuppressive medications. Local wound care and dressing selection are supportive measures but do not treat the underlying disease process!
Aggressive surgical treatment should generally be avoided. Debridement of active PG ulcers often triggers worsening of the lesion due to pathergy, where minor trauma causes the disease to progress. For this reason, surgical revision of the wound should be considered only by specialists, usually only after the inflammatory process is under control.
Local wound care should focus on protecting the wound, reducing pain, managing exudate, and preventing secondary infection.
Topical treatment
If the lesion is small and localized, it may sometimes be possible to achieve healing with topical therapy.
Potent topical corticosteroids (Group IV), such as clobetasol propionate (Dermovate), can be applied directly to the wound surface. The medication is usually applied at least twice daily until the ulcer has healed.
Another option is tacrolimus ointment 0.1% (Protopic). Tacrolimus is an immunomodulating medication and should be applied directly to the wound at least twice daily.
To prevent most of the ointment from being absorbed into the dressing, a hydrofiber dressing such as Aquacel can be used as an intermediate layer.
There is no clear consensus on whether topical corticosteroids or tacrolimus are superior. A common practical approach is to try topical corticosteroids for a few weeks, and if the response is insufficient, consider switching to tacrolimus.
If the ulcer does not respond within approximately 4 weeks or continues to enlarge, systemic treatment should be initiated.
However, dramatic improvement cannot be expected after only a few weeks. Early signs of treatment response include:
-
less inflamed wound edges
-
reduced pain
-
slower progression of the ulcer
If the ulcer has not yet decreased in size but appears clinically calmer and the patient reports less pain, it may still be reasonable to continue topical therapy.
Topical therapy is not considered standard treatment for most cases of PG, but it may be appropriate in mild or localized disease to avoid systemic treatment-related side effects.
PG sometimes responds paradoxically to topical steroids. We have had cases where the ulcer deteriorated when topical steroids were applied to the wound bed. That is rare, but something you need to be aware of.
Treatment of PG should always be managed by physicians experienced with this condition, including when topical therapies are used.

Figure 5. Intralesional steroid injections can be successful in smaller lesions/ milder cases of PG. Use the thinnest needle possible. We routinely use a 28-G needle to avoid unnecessary trauma to the wound edges, which may accelerate ulcer deterioration ( pathergenic effect). When we use intralesional treatment, we routinely combine it with topical steroid treatment. Image created with OpenAI.
Intralesional corticosteroid injections in pyoderma gangrenosum
In selected cases of small and localized pyoderma gangrenosum, intralesional corticosteroid injections may be used as an alternative or adjunct to topical therapy. This approach aims to deliver a high local anti-inflammatory effect while minimizing systemic side effects. In our clinic, we always use topical treatment as well when we consider intralesional injections.
The treatment is typically performed by dermatologists or clinicians experienced in managing PG.
The injections are usually placed in the inflammatory rim surrounding the ulcer, which represents the most active area of disease.
Evidence for the use of intralesional corticosteroids in PG is limited but supportive. Most published reports describe the successful treatment of localized PG with intralesional triamcinolone, either alone or combined with topical therapy. Several dermatology case series report rapid pain relief and ulcer stabilization, followed by gradual healing.
Because PG is rare, large controlled trials of intralesional therapy are lacking. Current international reviews and dermatology guidelines therefore consider intralesional corticosteroids a reasonable option for localized disease, particularly when systemic therapy can be avoided.
Remember that even a prick from a needle can trigger a pathergenic reaction, causing an increase in the ulcer. Therefore, we use the thinnest needle possible. We routinely use a 28-G needle for this. To make the injection easier for the clinician, use a low-volume syringe. You will struggle to squeeze the medication from a 10ml syringe through a 28G needle! Also, most patients with PG have a lot of pain- even a thin 28G needle will aggravate the pain. Numb the injection sites with numbing cream 30 minutes prior to the injections and consider providing systemic analgesics 45 minutes prior to the treatment.
The corticosteroid most commonly used is triamcinolone acetonide.
Typical concentrations used in dermatology practice:
-
5–10 mg/mL for delicate areas
-
10–20 mg/mL for thicker inflammatory borders
-
Most clinicians inject small aliquots (0.1–0.2 mL per injection point).
The injections are placed intradermally around the active border of the ulcer, usually spaced approximately 0.5–1 cm apart.
Total injected volume depends on ulcer size but is generally kept below 1–2 mL per session.
Injecting directly into the ulcer base is usually avoided; the goal is to treat the inflammatory rim where disease activity is highest.
Treatment frequency for intralesional injections:
Injections are usually repeated every 2–4 weeks, depending on the clinical response. Initially, we often start with weekly injections for the first two weeks, then move to two-week intervals.
Typical treatment course:
-
1–3 treatment sessions ( most lesions will require at least 3 treatment sessions! If the lesion healed with only one intralesional injection, most likely it wasn't PG!)
-
sometimes continued longer if the ulcer continues to improve
-
Early treatment response often includes:
-
rapid pain reduction
-
decreased inflammation of the wound edge
-
stabilization of ulcer size
Systemic treatment
Most patients with PG require systemic therapy. Currently, corticosteroids, cyclosporin, and TNF-alpha inhibitors are the most commonly used modalities.
Systemic corticosteroids:
The most commonly used first-line treatment is systemic corticosteroids. This is a relatively inexpensive treatment and is readily available in low-resource settings. Oral prednisolone at a dose of approximately 0.75–1 mg/kg/day is generally considered standard therapy. About 50% of the patients achieve complete wound healing with systemic corticosteroids. Similar results are seen with another first-line drug- cyclosporine.
When starting with systemic corticosteroid treatment, do not expect immediate results. Often, it takes about 4 weeks after the onset of treatment for a slight improvement to be seen. In some cases, there will be a significant improvement over several months before progress suddenly stalls. At this point, you will have to consider switching over to another treatment.
Some clinicians recommend maintaining high-dose treatment until the ulcer has clearly improved or healed. In other cases, gradual tapering may begin after several weeks, depending on the clinical response.
After healing, many patients require low-dose maintenance therapy for a period of time to reduce the risk of recurrence.
However, high-dose corticosteroids administered over several months will almost always lead to the well-known side effects of systemic corticosteroids and may include:
-
insomnia
-
restlessness and mood changes (sometimes psychosis)
-
weight gain
-
increased risk of gastrointestinal ulceration
-
metabolic complications
Never start with the maximum dose when starting with corticosteroids. When using prednisolone, for example, we routinely start with 20mg x 1 on days 1-5, 40mg x 1 on days 5-10, 60mg on days 15-20 before settling on the final dose. As mentioned above, we have, in a few cases, experienced psychosis in elderly patients receiving high doses of corticosteroids. You have to monitor your patients closely when using this treatment. Because high-dose corticosteroids are often the first-line treatment in many countries, we provide a detailed checklist below of factors to consider before and during treatment. This is especially important because we know that in many low-resource settings, clinicians who are not very experienced in treating PG may need to initiate and follow up on treatment alone due to limited options.
Steroid Safety Checklist
Patients treated with moderate to high doses of systemic corticosteroids for several weeks or months require structured monitoring to reduce the risk of treatment-related complications. One of many complications is, for example, steroid-induced diabetes.
Before starting corticosteroid therapy
Clinical assessment
-
Blood pressure
-
Weight / BMI
-
Diabetes risk factors
-
History of osteoporosis or fractures
-
Infection history
-
Medication review (especially NSAIDs or anticoagulants)
-
Laboratory tests
-
Complete blood count (CBC)
-
Electrolytes
-
Creatinine
-
Liver function tests
-
Fasting glucose or HbA1c
-
Lipid profile
Monitoring during treatment
Every 4–8 weeks (initially)
-
Blood pressure
-
Weight
-
CBC
-
Electrolytes
-
Creatinine
-
Liver enzymes
-
Glucose
Every 3–6 months
-
HbA1c
-
Lipid profile
-
Kidney and liver function
-
Patients should also be assessed clinically for:
-
edema
-
mood changes
-
sleep disturbances
-
infection signs.
Bone protection
For patients receiving corticosteroids for more than 3 months, most guidelines recommend:
-
Calcium 1000–1200 mg/day
-
Vitamin D 800–1000 IU/day
Patients at increased fracture risk should be considered for bisphosphonate therapy.
Risk factors include:
-
age >50 years
-
prednisolone ≥7.5 mg/day ( all of our PG patients receive a far higher dose than this)
-
previous fragility fracture
-
low bone mineral density.
Gastric protection
Routine proton pump inhibitor (PPI) therapy is not necessary for all patients receiving corticosteroids.
PPI prophylaxis should be considered if additional risk factors are present:
-
concomitant NSAID therapy
-
previous peptic ulcer disease
-
anticoagulant therapy
-
elderly patients on high-dose steroids.
Additional considerations
Monitor for:
Steroid-induced diabetes
-
Check glucose regularly
Hypertension
-
Monitor blood pressure at each visit
Ophthalmologic complications
-
cataracts
-
glaucoma
Cyclosporine
Another commonly used systemic treatment is cyclosporine (Sandimmun Neoral). What is most effective for PG: prednisolone or cyclosporine? There are very few randomized studies addressing this question. The best study so far is probably the STOP GAP trial from 2015, published in BMJ. The results from this multicenter study showed that both treatments have almost identical effectiveness.
The choice of medication, therefore, depends largely on which drug the patient is expected to tolerate best in terms of side effects.
It is recommended that patients be treated with cyclosporine (5 mg/kg/day) until the lesion(s) have healed. Treatment is then continued for an additional month at a lower dose.
Cyclosporine has well-known side effects. The most important risk is the risk of developing hypertension, and with treatment over several years, the medication may become nephrotoxic. Hypertrichosis, gingival hyperplasia, and polyneuropathy-like symptoms may also occur during cyclosporine therapy.
Patients treated with cyclosporine must therefore be carefully monitored.
When cyclosporine is used to treat pyoderma gangrenosum, most patients require treatment for only a few months, and the risk of serious side effects is therefore considered quite low.
We have only limited experience with cyclosporin ourselves. In our health region, we typically start with high-dose corticosteroids as first-line treatment. If the ulcer fails to respond or the patient experiences side effects, they are usually treated with a TNF-alpha antagonist such as Infliximab.
Figure 6: Mørk et al. published an article in the Journal of the Norwegian Medical Association describing three interesting cases of PG, all successfully treated with cyclosporin. The article is from 2000, but still highly relevant. Image copyright: Gro Mørk et al; Tidskriftet Den Norske Legeforeningen. Click on the image above to get to the article.
Figure 7. The STOP GAP study, conducted in 2015, is a multicenter study comparing the effectiveness of prednisolone and cyclosporine in the treatment of pyoderma gangrenosum. Both medications have approximately equal efficacy, but quite different side-effect profiles. Click on the image above to access the article.
Video 1. The STOP GAP study is a multicenter study from 2015 that compared the effectiveness of prednisolone and cyclosporine in the treatment of pyoderma gangrenosum. In this video, Professor Kim Thomas explains the study in more detail. The video also includes a case report of a patient who, for many years, was treated under the incorrect diagnosis of a “venous leg ulcer.”
Biologic therapies
In patients with severe or treatment-resistant PG, biologic therapies are increasingly used. In some centers, TNF-alpha inhibitors have become the first-line treatment. Unfortunately, these treatments are very expensive and therefore not a realistic option for many patients.
The most widely used agents are TNF-alpha inhibitors, particularly:
-
infliximab
-
adalimumab
Infliximab is the only biologic therapy that has been studied in a randomized controlled trial, and many clinicians consider it an effective treatment option, especially in PG patients with associated inflammatory bowel disease.
Be aware that these are complex treatments requiring significant experience with monitoring and following up the patients. Sometimes patients can develop antibodies to the drugs, making them ineffective. The monitoring of the treatment, therefore, also includes checking for the development of these antibodies.
Other, newer, biologic therapies targeting different inflammatory pathways are also being used in selected cases, particularly when conventional treatments fail. There are significant developments in this field of medicine, and new biologic therapies are being developed every year. However, the common denominator for all these treatments is that they are expensive and not available to all patients in resource-limited settings!
Other systemic treatment options
Other medications that are occasionally used include dapsone, methotrexate, cyclophosphamide, sulfapyridine, and tetracyclines. In the literature, one can find reports—most often individual case reports—of these medications being tried in various combinations. Hyperbaric oxygen therapy is also sometimes used in managing severe cases of PG
How should the PG wound itself be treated?
Especially in the active phase, it is important to treat the wound very gently. Necrotic tissue should be removed carefully. Extensive surgical debridement must be avoided, as it may lead to significant ulcer enlargement.
It is also debated whether any debridement should be performed before systemic treatment has been initiated. In most cases, however, the clinician is not aware that the wound is a PG ulcer and performs debridement as usual. At the next dressing change, one may notice that the wound has worsened or increased in size. At that point, it is important to step back and consider that the ulcer may be a pyoderma gangrenosum lesion.
PG ulcers often contain a lot of sloughy material. This can contribute to unfavorable microbial overgrowth, which may further worsen the situation. Although we generally try to avoid debridement of PG ulcers initially, it is still important to keep bacterial growth under control. Antibiotics are rarely indicated!
We have had good experience using Prontosan soaks, which are left on the wound for approximately 20 minutes. With regular use, this often helps keep the wound cleaner without the need for sharp debridement instruments.
Prontosan gel X has worked well in our hands. We apply it daily in a generous amount to the entire wound bed and cover it with a polyurethane foam or a superabsorbent dressing in high-exudate ulcers. The interesting part about Prontosan Gel X is that it does not cause maceration of skin edges, even though we are applying a moist wound product to an ulcer that often already has high exudate. Polymem Gel X is not very expensive.
We also recommend PolyMem dressings for PG ulcers. In our experience, PG ulcers tolerate this dressing well. It provides an autolytic debridement effect and appears to reduce pain. PolyMem rarely adheres to the wound and is usually painless to remove. At our clinic, we actually often combine Prontosan Gel X and Polymem. The latter already contains a surfactant, but when combining these two products, we get a "double surfactant" effect that, in our hands, works very well. Polymem, however, is quite expensive and will not be available in low-resource settings.
Some PG ulcers produce large amounts of exudate and require frequent dressing changes. The skin around PG ulcers appears to tolerate maceration very poorly. Macerated wound edges often lead to rapid enlargement of the ulcer area.
It is therefore important to prevent maceration by using:
-
skin barrier products
-
superabsorbent dressings
-
short dressing change intervals.

Figure 8. If we were to highlight a dressing for the treatment of PG, we believe it would have to be PolyMem. We have had good experience with this dressing, and based on case reports available online, several clinicians have reported favorable results when using PolyMem in PG ulcers. Again, there is no dressing that cures PG. However, choosing an appropriate dressing may help keep the wound cleaner and possibly reduce pain.
Some clinicians report good results with silver-containing dressings or honey-based products. When searching the literature or the internet, one can find case reports describing many different dressings that appear to support the healing process. Again, it is important to remember that systemic corticosteroid therapy (or other systemic treatment) is what ultimately determines whether the ulcer heals.
Be aware that PG sometimes reacts paradoxically to wound dressings that are otherwise considered safe in most other types of wounds. We have, for example, seen deterioration of some PG ulcers when treated with honey or iodine, whereas other PG ulcers improved with these dressings. This means that you have to monitor the ulcers closely at the start of the treatment to see how they respond.
In most cases, compression therapy is recommended for PG ulcers on the lower extremities. Because these ulcers are often very painful, the level of compression must be adjusted to what the patient can tolerate.
Once the ulcer is clean, negative pressure wound therapy (NPWT) may be considered. This treatment should be performed by clinicians experienced in both PG ulcers and NPWT. A prerequisite for starting NPWT is that the patient has been on systemic PG treatment for some weeks and that the ulcer is responding well. This recommendation may not be clearly described in the literature, but it reflects our clinical experience.
When the wound has developed satisfactory granulation tissue, split-thickness skin grafting may be considered. Important: trauma from harvesting the skin graft can trigger new PG lesions at the donor site. For this reason, grafting should be performed only when the disease is in a stable phase, meaning the patient has been on systemic medical treatment for some time.
In some patients, hyperbaric oxygen therapy may also be effective. It is important to remember that this option exists when treating PG patients whose ulcers do not respond adequately to other treatments.
Remember that patients with PG ulcers often require analgesic medication. In most cases, moderate analgesics such as paracetamol combined with codeine or tramadol are sufficient, although stronger opioids may sometimes be necessary.
Figure 9. We highly recommend this article for further reading. It provides an excellent overview of the differential diagnoses you will have to consider, as well as the possible treatment alternatives. Click on the image to get to the article.
Video 2. Alexandra Pyle works at the Welsh Institute of Dermatology. In this 2019 lecture video, she discusses a study of patients’ experiences with the diagnosis of pyoderma gangrenosum.
The presentation also provides a good summary of the side effects associated with long-term treatment with prednisolone or cyclosporine. Copyright: Global Alliance of Nurses in Dermatology / Alexandra Pyle / YouTube.
Video 3. A video from EWMA presents the story of a young woman with Crohn’s disease who developed pyoderma gangrenosum around her stoma. Note the severity of the pain experienced by the patient—not only in the ulcer itself but also in the surrounding skin. The patient was initially treated with systemic corticosteroids and later with biologic anti-inflammatory agents. Physicians at the Helsinki Wound Center also emphasize the importance of a multidisciplinary approach, including collaboration with the gastroenterologist to select a treatment that is compatible with the patient’s underlying disease. Copyright: EWMA / YouTube.
Video 3. Jerard Gardner is a pathologist specializing in dermatologic conditions. In this video, he provides an overview of pyoderma gangrenosum from a pathological perspective.
Copyright: Jerard Gardner / YouTube.
Video 4. Dr. Stanislav Tolkachjov, dermatologist at the Mayo Clinic in Rochester, discusses the study he conducted on postoperative pyoderma gangrenosum and explains how this condition is often overlooked by surgeons. Copyright: Mayo Proceedings / Stanislav Tolkachjov / YouTube.
References
General reviews and clinical overviews
-
Brooklyn T, Dunnill G, Shetty A, Bowden JJ, Williams JD, Griffiths CEM. Pyoderma gangrenosum: current understanding and future directions. Lancet. 2006;367:1817–1828.
-
Alavi A, French LE, Davis MD, Brassard A, Kirsner RS. Pyoderma gangrenosum: an update on pathophysiology, diagnosis, and treatment. American Journal of Clinical Dermatology. 2017;18:355–372.
-
George C, Deroide F, Rustin M. Pyoderma gangrenosum – a guide to diagnosis and management. Clinical Medicine (London). 2019;19:224–228.
-
Ruocco E, Sangiuliano S, Gravina AG, Miranda A, Nicoletti G. Pyoderma gangrenosum: an updated review. Journal of the European Academy of Dermatology and Venereology. 2009;23:1008–1017.
-
Braswell SF, Kostopoulos TC, Ortega-Loayza AG. Pathophysiology of pyoderma gangrenosum and implications for treatment. Journal of the American Academy of Dermatology. 2015;73:691–698.
Diagnostic criteria
-
Maverakis E, Ma C, Shinkai K, et al. Diagnostic criteria of ulcerative pyoderma gangrenosum: a Delphi consensus of international experts. JAMA Dermatology. 2018;154:461–466.
Histopathology and biopsy interpretation
-
Crowson AN, Mihm MC, Magro C. Pyoderma gangrenosum: a review. Journal of Cutaneous Pathology. 2003;30:97–107.
-
Schadt CR, Callen JP. Management of neutrophilic dermatoses. Dermatologic Clinics. 2015;33:429–440.
-
Binus AM, Qureshi AA, Li VW, et al. Pyoderma gangrenosum: a retrospective review of patients treated in tertiary care centers. British Journal of Dermatology. 2011;165:1244–1250.
Systemic treatment
-
Ormerod AD, Thomas KS, Craig FE, et al. Comparison of the effectiveness and safety of ciclosporin and prednisolone for pyoderma gangrenosum (STOP GAP): a randomized controlled trial. BMJ. 2015;350:h2958.
-
Thomas KS, Ormerod AD, Craig FE, et al. Clinical outcomes and quality of life in the STOP GAP trial for pyoderma gangrenosum. British Journal of Dermatology. 2016;174:1077–1084.
Biologic therapies
-
Brooklyn TN, Williams AM, Dunnill MG, Probert CS. Infliximab for the treatment of pyoderma gangrenosum. Gut. 2006;55:505–509.
-
Adams DR, Gordon KB, Devenyi AG, Ioffreda MD. Severe pyoderma gangrenosum treated with infliximab. Journal of the American Academy of Dermatology. 2005;52:510–514.
-
Marzano AV, Trevisan V, Lazzari R, et al. Targeted therapies in pyoderma gangrenosum. Dermatologic Therapy. 2020;33:e13219.
-
Kolios AG, Maul JT, Meier B, et al. Biologic therapies in the treatment of pyoderma gangrenosum. Journal of the European Academy of Dermatology and Venereology. 2021;35:197–205.
Topical and intralesional therapy
-
Ahronowitz I, Harp J, Shinkai K. Etiology and management of pyoderma gangrenosum: a comprehensive review. American Journal of Clinical Dermatology. 2012;13:191–211.
-
Feldmeyer L, Heidemeyer K, Yawalkar N. Topical therapy in pyoderma gangrenosum. Dermatology. 2016;232:515–521.
-
Callen JP. Pyoderma gangrenosum. Lancet. 1998;351:581–585.
Wound care and local management
-
Kirsner RS, Grossman ME. Management of pyoderma gangrenosum. Dermatologic Therapy. 2004;17:191–197.
-
Al Ghazal P, Körber A, Klode J, et al. Management of pyoderma gangrenosum: a systematic review. Journal der Deutschen Dermatologischen Gesellschaft. 2013;11:517–527.
-
European Wound Management Association (EWMA). Management of Pyoderma Gangrenosum. EWMA position document.
Corticosteroid safety and monitoring
-
Weinstein RS. Glucocorticoid-induced bone disease. New England Journal of Medicine. 2011;365:62–70.
-
Compston J. Glucocorticoid-induced osteoporosis: an update. Endocrine. 2018;61:7–16.
-
Saag KG, et al. American College of Rheumatology guideline for prevention and treatment of glucocorticoid-induced osteoporosis. Arthritis & Rheumatology. 2017;69:1521–1537.
































