Sickle cell leg ulcers
Content:
Diagnostics: Does the patient have SCD?
Diagnostic approach to the SCD ulcer
Practical treatment algorithm: Optimize the underlying sickle cell disease
Adjunctive and advanced therapies
Introduction
Abbreviations:
SCD: Sickle-cell disease
SCLU: Sickle- Cell Leg Ulcer
Sickle-cell disease (SCD) is the most prevalent genetic disease in the African Region. Despite its severe impact on children, it is still a neglected disease. Sickle cell disease is a genetic disorder that usually manifests in childhood and is characterized by anemia (a lack of healthy red blood cells), recurrent infections, and painful episodes. The defective hemoglobin molecules cause sickling (crescent shape) or clumping of red blood cells, resulting in vaso-occlusion, ischemia, inflammation, organ damage, and hemolytic anemia. SCD affects multiple organ systems, and there is no cure for SCD.
Leg ulcers are one of the most common cutaneous complications of sickle cell disease (SCD). They are typically chronic, very painful, slow to heal (months to years!), and prone to recur, and they often affect younger adults more than clinicians usually expect when thinking about chronic lower-limb wounds. If you have a patient with a leg ulcer and have no other good explanation for its etiology, get the patient checked for SCD! Modern reviews still emphasize that there is no universally accepted, disease-specific treatment protocol, and that management usually requires a combination of systemic sickle-cell optimization, meticulous wound care, pain control, and selected adjunctive therapies.
Sickle-cell leg ulcers are not simply venous ulcers in a patient who happens to have SCD. They are best understood as mixed hemolytic-microvascular-inflammatory wounds that often require simultaneous hematology and wound-care thinking. The treatments with the strongest practical day-to-day value are often the least glamorous: good assessment, pain control, gentle wound care, appropriate compression, nutritional optimization, and carefully chosen adjuncts such as arginine, L-glutamine, topical timolol (off-label), or zinc in selected patients.

Figure 1 Illustration shows some differences between a normal red blood cell and blood cells affected by the sickle-cell disease. It is not only the shape of the cells that are different but also, the hemoglobin within the cell that is altered. The sickle-shaped blood cells can easily block the blood flow of especially smaller blood vessels. Copyright: designua/Shutterstock
Epidemiology
The frequency of sickle-cell leg ulcers varies markedly by geography and population. Reviews describe the prevalence of SCD-related ulcers in adults as generally around 5%–10% globally, but with large regional differences and higher rates reported in some tropical regions and lower rates in parts of the Middle East, Europe, and North America. For example, one international study cited a prevalence of 10.8% overall, but 18.6% in Ghana, 3.5% in Italy, and 2.4% in the United States. Older cohort data also show that prevalence rises with age and is uncommon before age 10.
SCD is most prevalent among people of African descent. The global prevalence of SCD across all ages increased from 5.46 million to 7.74 million cases from 2000 to 2021 (WHO). A “sickle belt” has been described in Africa, stretching from the southern Sahara to the northern Zambezi, along an area between the 15th parallel north and the 20th parallel south; this area is also malaria-endemic.
The clinical effects of SCD vary significantly by phenotype. Leg ulcers are most often seen in patients with more severe forms of SCD.

Figure 2. A map showing the distribution of the prevalence of both Sickle-Cell Disease and b-Thalassemia (which is a related hemoglobin disorder). Copyright: https://caringcross.org/scd-bt-cure-project/ ( adapted from Williams and Weatherall, 2012)

Figure 2a. In many African countries, initiatives focus on raising awareness of sickle cell disease. Only a few focus specifically on treating SCD-related leg ulcers. The Sickle Cell Foundation of Nigeria states on its website that they treat over 6000 patients with leg ulcers annually. Click on the image above to get to their website. Image copyright: Sickle Cell Foundation Nigeria.
Pathophysiology
Sickle-cell leg ulcers are multifactorial. No single mechanism explains all cases. The current understanding centers on the interactions among hemolysis, nitric oxide depletion, endothelial dysfunction, microvascular occlusion, inflammation, local trauma, and, sometimes, venous hypertension/edema.
These ulcers characteristically occur in the gaiter area, especially around the medial and lateral malleoli. The reasons are practical and anatomical: this area has thin skin, little subcutaneous cushioning, a relatively marginal blood supply, exposure to trauma and friction from footwear, high hydrostatic venous pressure, and “watershed-like” vulnerability. In SCD, these local disadvantages, combined with systemic vasculopathy, make the malleolar area especially susceptible.
When the ulcers appear on the medial side of the leg, they are often misdiagnosed as venous ulcers. Many patients have some degree of venous insufficiency, but failure to detect that the wound is actually caused by SCD will delay the healing process!

Figure 3. Sickle cell-related leg ulcers often have a layer of yellow necrosis that needs to be debrided gently, preferably in several sessions. The edges may be slightly irregular or sometimes quite sharp. The ulcers are often located in the lower leg, but can present anywhere on the lower extremities. It is important to remember that sickle cell ulcers can mimic other ulcer types, and we should keep other aetiologies, such as tropical ulcers, pyoderma gangrenosum, and malignancy, in mind.
Clinical characteristics
Sickle-cell leg ulcers are usually:
-
Painful, often disproportionately so
-
Located around the malleoli
-
Debut often after a minor bruise or insect bite
-
Chronic and recurrent
-
Seen in younger adults than classic venous ulcers
-
Associated with surrounding hyperpigmentation, atrophic scarred skin, and sometimes mixed ischemic/venous features.
-
Often a yellowish fibrinous wound bed.
Compared with classic venous leg ulcers, they are often more painful, more refractory, and more tightly linked to systemic disease activity.
Diagnostics: Does the patient have SCD?
If the patient has no known SCD, you will need to initiate diagnostic testing for this disease. There are several options available:
-
Clinical suspicion:
SCD is usually suspected based on:
-
family history of SCD
-
ancestry from regions with high prevalence (sub-Saharan Africa, Middle East, India, Mediterranean, Caribbean)
-
typical complications such as:
-
vaso-occlusive pain crises
-
hemolytic anemia
-
stroke
-
acute chest syndrome
-
chronic leg ulcers.
-
-
Laboratory diagnosis:
Blood smear microscopy: A blood smear stained with Wright or Giemsa stain may reveal several characteristic abnormalities. However, blood smear diagnosis has several limitations. Microscopy cannot differentiate between SCD and β-thalassemia. Sickle cells may be rare and difficult to see. Artifacts during slide preparation can lead to false positives.
Sickling test (useful in low-resource settings): Blood is mixed with a reducing agent such as sodium metabisulfite. This reduces the oxygen tension, and if HbS is present, red cells sickle within minutes. It is an easy-to-perform, inexpensive, rapid test. Its limitation, however, is that it cannot distinguish between an SCD trait and the disease.
Hemoglobin electrophoresis remains the standard diagnostic test in many regions of the world. This technique separates hemoglobin types based on electrical charge.
High-performance liquid chromatography (HPLC) has, in many laboratories today, replaced electrophoresis, as it is even more precise.
Other diagnostic tools are Isoelectric focusing and DNA testing.
Diagnostic approach to the SCD ulcer:
The diagnosis of SCD ulcer is clinical. It is a combination of knowing the patient has SCD and the clinical presentation that may help us decide whether the ulcer is SCD-related. Beware of the pitfuls here. Just because the patient has SCD does not necessarily mean the ulcer is SCD-related! The diagnosis should not be made lazily! A patient with SCD can still have a venous ulcer, arterial ulcer, vasculitis, pyoderma gangrenosum, livedoid vasculopathy, infection, or a mixed ulcer.
Biopsies are not helpful for specifying whether an ulcer is caused by SCD, but they may help us rule out other conditions and malignancy.
Wound cultures are only done when infection is clinically suspected, rather than for routine colonization
Ankle-brachial index or other arterial assessment if clinically indicated
Duplex ultrasound to assess venous reflux/obstruction if clinically indicated
Basic blood work, including hemoglobin/hemolysis markers and nutrition-focused testing where relevant
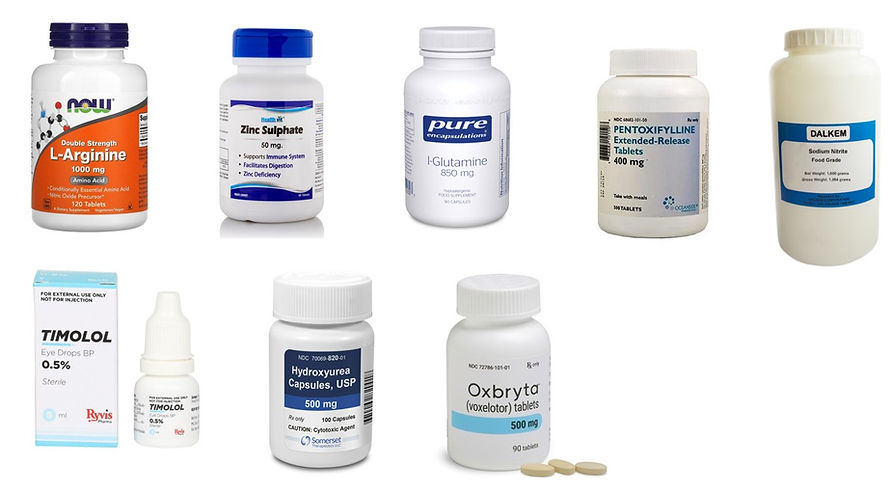
Figure 4. Treating SCD leg ulcers systemically presents us with several difficult choices. There is little evidence-based knowledge on this, and we lack clear guidelines for initiating treatment. In reality, no single treatment will work in every case, and you will often try one modality before switching to another after some months. We will discuss current systemic treatment options below.
Practical treatment algorithm: Optimize the underlying sickle-cell disease
In many cases, you will most likely not succeed in getting the ulcer to heal without treating the underlying causes systemically. Therefore, we focus on this aspect of the treatment. The preparation of the wound bed and the choice of dressings are not specific to SCD-related ulcers and are discussed at the end of this chapter.
Hydroxyurea
Hydroxyurea remains a key disease-modifying therapy in SCD, but its ulcer-specific effect is uncertain. Earlier reviews noted no clear proof that it reliably heals sickle-cell leg ulcers, although it remains important for overall sickle-cell control in appropriate patients. It should therefore be viewed as systemic SCD management, not as a proven ulcer-healing drug. In fact, hydroxyurea may actually delay wound healing. Therefore, the indications for initiating hydroxyurea should be discussed with a hematologist experienced in SCD ulcers beforehand.
Chronic transfusion
Chronic or repeated transfusions have been used in severe or refractory cases, especially when the ulcer is part of severe systemic disease, but there is no strong controlled evidence demonstrating consistent ulcer-healing benefit. It may still be reasonable in selected patients in collaboration with hematology.
L-glutamine
L-glutamine (Endari) is approved in SCD to reduce acute complications, not specifically for the treatment of leg ulcers. The rationale is to reduce oxidative stress and improve red-cell redox balance. It can be considered part of broader SCD optimization, but readers should understand that ulcer-specific evidence is indirect. The FDA label recommends oral dosing twice daily by weight:
-
<30 kg: 5 g twice daily
-
30–65 kg: 10 g twice daily
-
>65 kg: 15 g twice daily
-
Each dose is mixed with a cold/room-temperature beverage or soft food.
Oral Arginine
Arginine is interesting because SCD is associated with low nitric oxide bioavailability and increased arginase activity. However, there is no standardized dose specifically for sickle-cell leg ulcers. In SCD studies more broadly, oral dosing of 0.1–0.2 g/kg/day has been used, usually divided into 2–3 daily doses. For an adult, that often translates to about 6–10 g/day, for example, 3 g three times daily, but this should be presented as off-label adjunctive practice rather than evidence-based ulcer dosing. Small studies and physiologic work suggest arginine and citrulline can increase nitric oxide production in SCD, but robust ulcer-healing trials are lacking.
Practical caution: oral arginine can cause gastrointestinal upset and may lower blood pressure. It should be used cautiously in patients with significant hypotension or advanced renal disease, and ideally in consultation with hematology if prolonged high-dose use is planned.
Zinc sulphate
Zinc is one of the oldest metabolic treatments discussed for sickle-cell leg ulcers. Zinc deficiency is common in SCD and may impair immune function, collagen synthesis, epithelialization, and antioxidant defenses. The classic randomized trial by Serjeant and colleagues used zinc sulfate 220 mg three times daily, which corresponds to about 50 mg elemental zinc per capsule, or approximately 150 mg elemental zinc/day total. Reviews continue to cite this study as showing faster ulcer healing with zinc.
Practical dosing options
-
Historical trial dose: zinc sulfate 220 mg three times daily
-
More conservative modern practice: 220 mg once or twice daily in selected patients, especially if deficiency is suspected
-
Important caution: long-term high-dose zinc can cause copper deficiency, anemia, and neutropenia, so prolonged treatment should be monitored. Zinc is best framed as an adjunct, not as a sole therapy.
Pain management
Pain is central in these ulcers and is frequently undertreated. Reviews emphasize that the ulcers are often very painful and that poor pain control reduces tolerance for dressing changes, compression, and debridement. Practical measures include:
-
procedure-related topical anesthesia where appropriate
-
systemic analgesics tailored to the patient
-
consideration of neuropathic pain agents when the pattern suggests a neuropathic contribution
-
improved edema control and wound inflammation control, which often reduces pain indirectly.
Adjunctive and advanced treatment options
Topical timolol (off-label) b-blokker drops
This is one of the most practical adjuncts to discuss because it is inexpensive, accessible, and easy to apply, but readers should understand that its use in sickle-cell ulcers is off-label and based mainly on evidence from other chronic wounds. Reviews of timolol in wound healing describe improved re-epithelialization, modulation of inflammation, and wound maturation, with 0.5% timolol being the most commonly reported topical wound formulation, usually applied once or twice daily.
Why timolol might help:
Keratinocytes, fibroblasts, and endothelial cells express beta-adrenergic receptors. Blocking these receptors appears to enhance keratinocyte migration, support angiogenesis, and help chronic wounds exit a stalled inflammatory state.
Which preparation to use
In practice, most clinicians use commercial ophthalmic timolol maleate solution, usually:
-
0.5% eye drops are most commonly
-
0.25%, sometimes when caution about absorption is desired
-
This means you usually do not need to compound the drug yourself. The commercially available ophthalmic solution is already sterile and easy to dose.
Practical dosing
There is no single universal wound dose, but common published regimens include:
-
1 drop of 0.5% timolol per 2 cm² of wound area once daily, then cover with dressing
-
Some studies/case series used 1 drop every 2 cm² of wound edge weekly under compression
-
Allow about 30–60 seconds for contact.
-
Cover with a non-adherent silicone contact layer or a hydrofiber
-
Add a suitable secondary dressing, such as foam, depending on the exudate.
-
Repeat once daily. In selected refractory cases, some clinicians use twice-daily dosing, but once-daily is the more conservative starting schedule.
Reassess after 4–6 weeks. If there is a clear reduction in pain, edge advancement, or size, treatment may be continued until epithelialization.
Safety
Topical wound use can lead to systemic absorption comparable to ophthalmic use in at least some settings. Be careful in patients with:
-
asthma or bronchospasm
-
bradycardia
-
heart block
-
marked hypotension
Be more cautious with large ulcers or twice-daily use.
Topical sodium nitrite / nitric-oxide donor therapy
This is one of the most biologically rational experimental treatments because sickle-cell leg ulcers are linked to nitric oxide depletion. In a phase 1 dose-finding study, topical sodium nitrite cream was tested in concentrations from 0.5% to 2.0%. Higher concentrations were associated with increased peri-wound blood flow, reduced pain, and dose-dependent ulcer shrinkage; complete healing occurred in some patients receiving 1.8%–2.0% cream. The authors concluded that 2% cream was suitable for further clinical trials.
At present, there is no widely marketed commercial topical sodium nitrite cream for wound care. The formulations used in studies of sickle-cell leg ulcers have generally been research formulations prepared in hospital pharmacies or research centers, rather than commercial products. Currently, one would have to make this themselves if intending to use this in patients. Be aware that sodium nitrate topical ointment is not currently FDA-approved.
However, if we have a patient in a desperate situation where other treatments have failed, we would need to consider all options. Sodium nitrite powder is readily available at most pharmacies. Some hospital pharmacies can easily make this for you. Hypothetically, if we were to prepare a sodium nitrate ointment with a 2% strength, we would do the following:
Step 1. Dissolve sodium nitrite powder in sterile water or saline to produce a 20–40% solution (often ~30%).
Example:
-
30 g sodium nitrite
-
sterile water to 100 mL
This yields a 30% solution.
Step 2 — incorporate into ointment base
Add about 4–5% of this solution to a petrolatum base to produce the final topical formulation.
Example calculation for 2% sodium nitrite cream:
Final target:
2 g sodium nitrite per 100 g ointment
-
6.7 g of 30% sodium nitrite solution
-
93.3 g petrolatum or Aquaphor
Mix thoroughly until homogeneous.
This yields approximately 100 g of 2% sodium nitrite ointment.
In most studies, the ointment was applied at least twice weekly, sometimes daily. Note that there are important safety considerations. Topical sodium nitrite is generally well tolerated in studies, but several precautions apply:
Possible risks:
-
hypotension if absorbed systemically
-
methemoglobinemia (rare)
-
local irritation.
Therefore:
-
avoid very large application areas initially
-
Monitor patients with severe anemia or cardiovascular disease.
Pentoxifylline
Pentoxifylline improves RBC and leukocyte deformability, potentially decreasing blood viscosity, platelet aggregation, thrombus formation, and plasma fibrinogen levels. This increases microcirculatory flow and tissue oxygenation, making it a good modality for treating leg ulcers in patients with sickle cell disease. One case report reported that 400 mg of oral pentoxifylline, taken three times a day, completely healed a leg ulcer in a patient with sickle cell disease within 3 months. In nine RCTs involving 572 patients, pentoxifylline combined with compression bandages improved ulcer healing. The 2014 clinical practice guidelines of the Society for Vascular Surgery and the American Venous Forum recommend the use of pentoxifylline for the treatment of long‐standing or large VLUs. As venous insufficiency is often present in SCD patients, pentoxifylline may be a good treatment option for them.
Voxelotor
In May 2024, NICE recommended voxelotor for patients with SCD (NICE, 2024). Voxelotor has been shown to inhibit polymerization and reduce hemolysis.
A trial from 2019 examined the safety and efficacy of voxelotor administered at two doses, 1500mg and 900mg. In this trial, 13 of the 274 enrolled patients had an active leg ulcer, 33 reported a history of leg ulcers, and 9 patients developed a leg ulcer during the trial period. More than 70% of the patients on voxelotor had their leg ulcers heal by week 24, and these were associated with an increased hemoglobin and reduced hemolysis. The number of patients included with leg ulcers was small, but this updated NICE guidance on the availability of voxelotor is encouraging for future patients with SCD-related ulcers. However, since ulcer healing itself was not a primary endpoint in these trials but rather a secondary analysis, it should be seen as a disease-modifying therapy that may indirectly improve ulcers, rather than a dedicated ulcer treatment.
Photobiomodulation and photodynamic therapy
Recent wound literature suggests that photobiomodulation and, in some centers, combined photodynamic therapy plus photobiomodulation, may help chronic wound healing and pain. For sickle-cell ulcers, the evidence remains preliminary and not standardized enough to recommend a specific protocol for a general readership, but it is reasonable to mention it as an emerging adjunct.
Platelet-rich plasma (PRP)
PRP has been explored as an adjunct in chronic wounds because it may provide growth factors that support angiogenesis and granulation. In sickle-cell ulcers, evidence is limited and not mature enough to support a standardized regimen, but it may be considered in refractory cases in specialized centers.
Negative pressure wound therapy (NPWT)
NPWT can be considered in selected larger or more complex ulcers when exudate control and granulation support are needed, but pain, ischemia, and tolerance must be considered. The evidence is not specific or strong enough to make it first-line.
Skin grafts, dermal matrices, and bioengineered skin
Advanced closure methods such as split-thickness skin grafting, dermal matrices, and bioengineered skin substitutes have all been used. These can work, but graft failure is more common than in ordinary venous disease because the underlying tissue is often ischemic and inflamed. They are best reserved for selected, well-prepared wounds after systemic and local optimization.
Hyperbaric oxygen
Hyperbaric oxygen has been reported in case-based or small-scale experience, but it remains experimental in this setting and should not be presented as standard care.
LMWH / anticoagulation
Because sickle-cell ulcers may involve microvascular thrombosis, low-molecular-weight heparin has occasionally been considered in refractory cases, especially when the ulcer looks livedoid or thrombotic. However, there is no good evidence to support routine LMWH for sickle-cell leg ulcers, and the bleeding risk and daily injections are important downsides. It should be reserved for highly selected cases or another clear indication for anticoagulation.
Other experimental systemic agents that have historically been studied
The literature includes small trials of therapies such as arginine butyrate, isoxsuprine hydrochloride, and L-carnitine, as summarized in treatment reviews, but these are not mainstream wound-clinic options today.
Wound bed preparation
Cleansing
Use simple cleansing with normal saline or another non-cytotoxic solution. Routine harsh antiseptic scrubbing should be avoided.
Debridement
Debridement should usually be gentle and conservative. Reviews recognize that these ulcers are ischemic, painful, and prone to worsening if over-traumatized. Suitable approaches include:
-
Conservative sharp debridement, repeated gentle debridements at each session, is usually better than a single aggressive debridement.
-
autolytic debridement
-
enzymatic debridement, where available
Avoid aggressive repeated excision in a poorly perfused, very painful ulcer unless there is a clear surgical indication.
Dressings and moisture balance
As with other chronic wounds, use dressings based on the wound bed:
-
hydrogel for dry wound beds
-
hydrofiber/alginate for more exudative ulcers
-
foam as a secondary absorbent layer
-
Super absorbent secondary dressings for highly exudative ulcers
-
non-adherent silicone contact layers when the wound is painful or fragile
-
Antimicrobial dressings such as iodine-, PHMB-, or silver-containing products may be reasonable when bioburden is a concern. SCD-related ulcers are often colonized, and especially at the onset of the treatment, some weeks of treatment with antimicrobial dressings may be indicated.
-
The goal is a stable, moist environment without maceration.
Compression therapy
Compression is often underused in sickle-cell ulcers because clinicians worry about ischemia. Reviews nonetheless note that many patients also have venous stasis, edema, or mixed disease, and compression may help when used thoughtfully.
Practical approach
-
Ischemia is rarely an issue in younger patients with SCD, and most patients will tolerate moderate compression therapy.
-
begin with light to moderate compression, often around 20–30 mmHg
-
consider short-stretch bandaging or adjustable wraps
-
escalate gradually depending on pain and tolerance
Figure 5. Most countries have national guidelines for the treatment of SCD. Click on the image above to get to the National Guidelines for the Management of Sickle Cell Disease in Kenya, for example. Image copyright: https://africasicklecell.org/
Recurrence prevention
Recurrence is common. Long-term care should include:
-
edema management and maintenance compression when appropriate
-
protection from trauma and footwear friction
-
early treatment of minor skin breaks
-
skin moisturization
-
Ongoing systemic sickle-cell optimization.
Figure 6. We found this article in Intech Open useful for further reading and alternative views to our own chapter. Click on the image above to get to the article.
Figure 7. Click on the image above to get to a PDF patient information brochure about SCD leg ulcers provided by LegsMatter.org. You could adapt this to your own clinical setting. Image copyright: legsmatter.org
Figure 8. The WHO has several documents concerning intervention packages for SCD. Click on the image above to get to their website. Image copyright: WHO
References
-
Monfort JB, et al. Leg Ulcers in Sickle-Cell Disease: Treatment Update. 2020.
-
Minniti CP, et al. Leg Ulcers in Sickle Cell Disease. 2010.
-
Martí-Carvajal AJ, et al. Interventions for treating leg ulcers in people with sickle cell disease. Cochrane update, 2021.
-
Serjeant GR, Galloway RE, Gueri MC. Oral zinc sulphate in sickle-cell ulcers. Lancet. 1970.
-
FDA / Accessdata. Endari (L-glutamine) Prescribing Information.
-
Catella J, et al. Controversies in the pathophysiology of leg ulcers in sickle cell disease. 2024.
-
Jackson TA, et al. Leg ulcers are indicators of systemic dysfunction in sickle cell disease. 2024.
-
Granja PD, et al. Leg ulcers in sickle cell disease patients. 2020.
-
Leigh R. Wound healing in sickle cell leg ulcers. Wounds UK, 2024.
-
Minniti CP, et al. Topical sodium nitrite for chronic leg ulcers in patients with sickle cell anaemia: phase 1 dose-finding safety and tolerability trial.
-
Lyle RE, et al. The Use of Timolol for Wound Healing—A Review. 2024.
-
Vestita M, et al. Topical 0.5% Timolol for Chronic Refractory Wounds. 2017.
-
Rai AK, et al. Efficacy of topical timolol versus saline in chronic venous ulcers. 2020.
-
Braun LR, et al. Topical Timolol for Recalcitrant Wounds. 2013.
-
Gallegos AC, et al. Absorption and Safety of Topically Applied Timolol for Chronic Wounds. 2019.
-
Marealle AI, et al. Arginine and citrulline supplementation increases whole-body NO production in children with sickle cell disease. 2018.
-
Gomaa DA, et al. L-arginine trial in sickle cell disease. 2025.




























