Offloading diabetic foot ulcers

Figure 1. Whenever we treat a patient with a diabetic foot ulcer, we have to think about how we want to offload the affected area of the foot. Off-loading is the most important aspect of treating diabetic foot ulcers. It is useful to have a toolbox of quite simple aids to achieve this. A) Customized shoe inserts B) Adhesive wool felt pads C) Soft-cushioning foam D +E) Silicone putty F) Cushioning toe orthotics G) Special shoes with adequate width and height, especially in the toe area.
Off-loading diabetic foot ulcers is the most important aspect of your treatment plan, and your choice of dressing is only of secondary importance. Paradoxically, many caregivers think the opposite and believe that they can skip the off-loading part if they have a good dressing. At our wound clinic, none of the referred patients have anything on the foot to off-load the ulcer! Again ( and we will repeat this to the point of being intrusive!): when you are treating a diabetic foot ulcer, consider first how you will off-load it. Only then make a plan for which dressing to use.
Remember that when we want to off-load a diabetic foot, we want to do this in such a way as to allow the patient to keep walking with both feet. You may ask whether it wouldn\t be more effective to give the patient a pair of crutches and ask them not to touch the ground with the affected foot. Yes, this would undoubtedly provide the best off-loading. In the early phase of an infected and out-of-control diabetic foot ulcer, we certainly advise using crutches as well to off-load as well as possible until we see some improvement. But advising the patient to use crutches for a more extended period is not feasible in the long run. Remember that most diabetic foot ulcers will take many months to heal. Do you expect the patient to walk with crutches for months on end? Therefore we have to achieve off-loading while allowing the patient to ambulate as they wish. The most effective method to off-load a diabetic foot is to use either a cast ( total-contact-cast TTC) or a special diabetic walker orthotic. Because this is quite a drastic measure, we usually only use this in more severe cases or when more simple aids do not seem to be adequate.
It is not enough to simply provide the patient with customized shoe insoles in most cases. These insoles can be helpful to prevent ulcers from developing but have a limited role in the treatment of active diabetic foot ulcers. Adhesive wool felt is a valuable tool for off-loading diabetic foot ulcers regardless of their anatomical location. This is the main form of off-loading at our clinic that we use. We usually try this for a few weeks - if it doesn't seem to provide enough off-loading, we use a diabetic walker orthotic ( or a total-contact-cast). Also, in many western countries, too few patients are treated with TTC or walker orthotics. Some diabetic foot ulcers will simply not heal unless you use this off-loading.
In the following subchapter, we will look at some off-loading techniques.

Figure 2 Using aids like walkers and crutches is a useful supplement to off-load the diabetic foot. However, they are never enough as a "stand-alone" tool. You will have to protect the ulcer from pressure in other ways too. We cannot expect the patient to use a walker or crutches for months while the ulcer slowly is healing. Our goal when applying off-loading principles is to keep the patient walking on both feet. In critical situations, for example, a severely infected foot or following surgery on the foot, we can ask the patient to keep the affected foot off the ground for a few weeks using crutches, a walker, or a wheelchair. image copyrights: left: cutches4africa.com,; right: Shutterstock
Removing hyperkeratosis (callus) from around the wound edge
Diabetic foot ulcers have the peculiarity that they develop very thick skin ( hyperkeratosis or callus) around the edge of the wound. We do not know why this happens especially in patients with diabetes. What we do know,however, is that this thick hard skin in itself presents a pressure risk and can lead to further breakdown of tissue beneath it. Removing these thiock edges is an important part of the off-loading treatment plan! The thickened wound edges also prevent the wound from healing as they cause the wound edge to go into a state of dormancy. When we debride the wound edges we activate them to start the healing process.
There is absolute agreement in the specialist community that the hard hyperkeratotic edge of the ulcers needs to be debrided. We often use a scalpel ( no. 15 blade is perfect) or a ringcurette for this procedure. remove the thick tissue until you get to a layer where you may encounter slight bleeding. Do not worry if it starts to bleed a little - this usually heals very quickly. Very often the thickened edge builds up again in the course of only a few days and very often you have to debride the wound edges repeatedly, for example every week. Many diabetic patients who have plantar ulcers also have some degree of sensory neuropathy and very often the removal of hyperkeratotic edges is completely painfree.

Figure 3 All these diabetic foot ulcers have in common that they have the characteristic hyperkeratotic wound edges. All these ulcers need a thorough debridement of the wound edges!
Video 1 An example of the debridement of a minor diabetic foot ulcer. The video shows how to debride the ulcer edges themselves and the hyperkeratotic skin surrounding the ulcer. We find that a sharp ring curette is the best tool for this. It is not uncommon to get small bruises when debriding, which can bleed ( as seen in the video). These are usually not a problem and normally heal well. Copyright: woundcarewindow
Off-loading using adhesive wool felt.
One of the best pieces of advice we can give you is to get a hold of self-adhesive wool felt. It seems incomprehensible to us that we managed to treat diabetic foot ulcers many years ago when we didn't have this fantastic tool. Podiatrists have a long tradition of using adhesive wool felt for off-loading. Still, paradoxically it took a while before this was introduced to most wound care clinics in western countries. The best-known brand is Hapla felt. It has a very good adhesive side which adheres well to the skin but is gentle at the same time. Although the adhesive is powerful, we very rarely ( basically never) have seen allergic reactions to the product, even after months of use. The wool felt can be left in place for up to 14 days while the dressing is changed at regular intervals. Be aware that depending on where the felt is placed, it will gradually lose its protective properties as it gets compressed under daily pressure - it gets worn out. In other words- you cannot simply place a felt pad around the ulcer and hope that it will last for 14 days. Depending on where the ulcers are located on the foot, the walking pattern of the patient, and their body weight, the felt can sometimes get worn out within a few days.
To ensure that the felt sits better, it is usual to fixate it with a special fabric tape - in the case of Hapla products, this is called Hapla tape or Hapla band to be even more correct.
Adhesive protective felt comes in various thicknesses. For off-loading diabetic foot ulcers, anything less than 5 millimeters in thickness does not provide enough protection. If you are using a very thick felt ( for example, 12 millimeters), this may feel like a lump in the shoe. Very often, we start off using felt with a 7-millimeter thickness. If the ulcer responds well, we keep using this thickness during the entire treatment. If the ulcers are not responding as expected, we increase the thickness or consider using a total contact cast or a walker boot orthotics.
The main problem with adhesive protective felt is that it is pretty expensive. Sheets of Hapla felt are usually sold in a 45cm x 22,5 cm size, and a single sheet often sells for around 20 US Dollars. Depending on the size of the ulcer that needs to be protected, a single sheet may be sufficient to treat a foot for several months - so in the long run, it is not that expensive. Initially, however, when you are buying several sheets of felt to have in stock, this will obviously feel expensive. If you cut the felt clever to have as little as possible waste, a felt sheet will take you a long way.
Many patients in Africa may not be able to return to your clinic for a follow-up after a week or so. Knowing that the protective felt will get worn out over a week, you will have to teach the patient how to change and reapply the felt at regular intervals. Our tip is to pre-cut the felt, making it easy for the patient to reapply. Make sure to give them a thorough explanation of how important it is to off-load the wound using the felt to ensure better compliance. On a side note: wool felt is quite difficult to cut with regular scissors- we advise you to have a strong pair of scissors at hand.
Adhesive wool felt is not available in many African countries. It is sold online at some shops providing podiatry equipment, and you can obtain it online via eBay or Amazon, for example.

Figure 4 Hapla Felt and Hapla Band are some of the most popular and widespread brands of this type of product. The wool itself is self-adhesive but should be re-inforced with Hapla Band, a strong self-adhesive tape.

Figure 5 It is generally advised to cut the opening in the felt in the shape of a horseshoe, and it is thought that this is better for the microcirculation around the wound. In this example, the edges of the wool felt have not been beveled. In Figure 7, you will see an example of how the felt should be cut around the edges to avoid causing unnecessary pressure at the edge of the felt.

Figure 6 Another example using wool felt. This is an ulcer secondary to the amputation of the great toe. We have placed U-shaped self-adhesive wool felt around the ulcer and re-inforced it with hapla Band. The wound itself is treated with a silver-coated contact layer and a foam dressing over that. The dressing is then held in place with an easy-to-remove adhesive tape. This patient kept the wool felt in place for two weeks at a time, while the dressing was changed every third day.

Figure 7 If the wound does not respond to small wool felt as offloading; you can try placing wool felt over a larger area, even the entire sole, as shown here. Note how the foot's arch is first filled with a piece of wool felt before the large wool felt piece is placed over the entire sole. This will build so much height that the patient will often not fit into regular shoes. If you are using a Walker boot or a total contact cast, you should pad the foot in this manner. Notice that the podiatrist who made this did not cut the opening around the ulcer in a U-shape. When applying wool felt over large areas of the foot, you do not necessarily have to cut the opening in a U-shape. Also, notice the beveled edges of the felt to prevent unnecessary pressure at the felt edges.
Video 2 Demonstration of advanced wool felt offloading on a foot. In this example, a smaller bit was again placed in the arch of the foot, and then the entire foot was covered with two plates of wool felt. We rarely use such thick layers with wool felt but want to show you that there are many ways to do this.
Figure 8 Some shops selling podiatry equipment in South Africa also supply protective adhesive felt. One of these shops is Leoto Podiatry Supplies. Click on the image above to get to the page with protective felt. Om såret ikke ser ut til å respondere på en enkel filtavlastning slik som er vist i Fig.4 er det ofte behov for mer omfattende filtavlastning. Her er det brukt en teknikk hvor det legges filt på hele fotsålen. Legg merke at det først er limt en filt bit under fotbuen for å utjevne den fordypningen her. Over dette er det limt en filt plate som dekker hele fotsålen. Dette er en type avlastning en for eksempel bruker i en total contact cast ( TCC)
Offloading ulcers on toes using silicone
Ulcers on the toes of diabetic patients usually arise due to mechanical pressure secondary to deformities ( motoric neuropathy) of the toes. Some of the most common deformities are hammertoes and claw toes. For preventive measures, padded sleeves for toes can be effective, but these sleeves are usually not enough once an ulcer has already developed. In many cases, using self-adhesive wool felt can be helpful to offload and protect the end of the toes.
Many caregivers are unaware that making custom-made silicone orthotics is easy and effective for offloading toes. This is a skill podiatrists know more about, but anyone treating diabetic foot ulcers should have basic knowledge about how to make a simple toe orthotic. If you have a podiatrist readily available, you can, of course, refer the patient there to get this made.
It takes about 15 minutes to make a silicone orthotic. The technique involves mixing two silicone components in your hand and then molding the blend around the affected toes. The mixture hardens within a few minutes. The freshly made orthotic has to harden further a few hours before it can be applied to the foot. In some cases, the silicone orthotic only needs to be worn during the day when the patient is ambulating. In other instances, the orthotic should be worn day and night depending on the deformity of the foot. The orthotic can be washed with normal water and soap. It usually needs to be replaced every third month. A silicone orthotic is a cost-effective method for offloading pressure-prone areas around toes- each orthotic will only cost about 1-2 US dollars.

Figure 9 All these diabetic ulcers of the toes have in common that they need immediate offloading. Which dressing we use on the ulcers is less relevant, the offloading part is the crucial part of the treatment. We can use self-adhesive wool felt here. Alternatively we can make a custom made silicone orthotic.

Figure 10 There is a wide assortment of silicones for orthotics available. One of the most popular brands is Fresco from Italy. Their assortment has many different varieties, some are more hard than others. For beginners we recommend Duo 10-A and -B which are easy and forgiving to work with. Equal amounts of Duo-A and Duo B are mixed together by hand and molded around the affected toes. The silicone hardes within minutes. The image on the right shows a finished silicone orthotic.
Video 3 An introduction to offloading using two-component silicones by FRESCO

Figure 11 This patient has severe sensory neuropathy in both feet. In addition, she has motoric neuropathy with hammertoes as a result. Over several years she went with recurrent ulcers on the end of her toes due to mechanical pressure from shoewear. Within a few weeks of using her custom-made silicone orthotics, she was without ulcers. These perfectly made orthotics were made by a podiatrist. Because this patient has sensory neuropathy, she does not feel any discomfort from wearing the orthotic all day long. Since the silicone is so soft, also patients with intact sensory function usually tolerate these orthotics very well. These orthotics need to be renewed regularly- usually about every third month. Our patient in this picture will have to use this type of orthotic lifelong because her ulcers will recur quickly if she does not offload the toes.
Offloading with prefabricated "half shoes."
Few caregivers are aware of this option for offloading the forefoot or hindfoot. These types of shoes are also called anterior wedge shoes/ posterior wedge shoes or forefoot/hindfoot offloading shoes. There is some discussion about how effective they are. In our opinion, they are a helpful alternative for patients with plantar ulcers of moderate severity. Suppose you have a patient where you are very worried about the prognosis; a Walker boot will provide even better offloading. A wedge shoe may be a good alternative for ulcers where you think the situation is under control. Most patients find that a wedge shoe is a very acceptable alternative for long-term use instead of a walker boot. For optimal offloading, we recommend that you use adhesive wool felt or other padding material in addition to the wedge shoe.
When resources are scarce, it is easy to make a wedge shoe out of a regular shoe that has a fairly thick sole. The front 1/3 or hind 1/3 of the sole can be removed using a handsaw. If a local shoemaker is consulted, they will easily be able to make an adequate wedge shoe for an acceptable price.

Figure 12 In our opinion, wedge shoes are not used as widely in diabetic foot care as they should be. Most patients find these to be a very acceptable alternative for offloading. For a plantar ulcer on the hind foot a posterior offloading wedge shoe is used. For a ulcer under the forefoot area a forefoot wedge shoe is used. With some improvisation these type of shoe can be made out of other prefabricated shoes.

Figure 13 Most local shoemakers have the tools and skills to make some sort of offloading shoe from a regular shoe. . This could be a wedge shoe or simply a shoe with a modification of the innersole. A regular shoemaker is obviously not a specialized orthotist, but if we can convey our aims with an improvised offloading shoe, the result can be more than adequate. Image copyright: Eyatalmsut, Wikimedia commons.
Offloading orthotics that go up to ankle level
If the patient has tried adhesive wool felt and maybe even a wedge shoe for some weeks without seeing improvements in the ulcer, then more "drastic" offloading measures have to be taken. An excellent choice for offloading is a special boot called a walker boot. The higher the boot sits up on the leg, the better it will unload, provided that the boot fits properly.
Why does an orthotic boot offload better than a well-cushioned shoe? Firstly, these boots have a large surface area in the sole area. These boots are pretty enormous, thus spreading the pressure out over a large surface area. When the boot fits snuggly higher up on the leg, some pressure is also transferred to the leg. Combining these two factors may reduce the plantar pressure by about 30-40%, which is usually sufficient to make the ulcer heal. As with wedge shoes, it is recommended to pad the foot with adhesive wool felt.
As we mentioned earlier - the higher the boot sits on the leg, the better the offloading effect is. A boot that goes about as high as a mountain boot will give better offloading than a regular shoe. However, in our opinion - if there is a need for a walker boot, then it should preferably be a long boot that sits high up on the leg. So which patients may benefit from a shorter boot that only is ankle-high? In our opinion, this short version of a boot may be an alternative for patients for whom the longer version is not acceptable.
Walker boots are costly. The shorter versions often cost almost the same as long boots. For many African patients, the price of a walker boot makes this an offloading aid they cannot afford. Be aware, however, that prices vary enormously between manufacturers. Even in Europe, wholesale prices can vary between 50 - about 300 US Dollars for a walker boot. Buying them in bulk directly from China via channels like Aliexpress may be a good alternative. Walker boots can also be refurbished and used for several patients. A shoemaker can easily make a new insole for a Walker boot.

Figure 14 Ankle height walker boots do not provide as much offloading as a boot that goes higher up on the leg. However, these shorter versions may be a solution for patients for whom a long boot is not acceptable.
Offloading orthotics that go high up on the leg ( Walker boots)
This type of boot is generally seen as the next best offloading aid next to a total contact cast (TCC). As we mentioned earlier, if the boot sits nicely on the leg, it may reduce the plantar pressure by about 40%, possibly even more. To achieve this, the boot has to sit snuggly, but it should not be too tight either. Velcro bands usually adjust the boot to tighten the boot around the leg. The most modern offloading boots have air-filled cushions lining the inside of the boot. These can be inflated by a pump and thus ensure a perfect fit. The cushions have a safety valve so that it is not possible to have too much pressure in the air cushions.
At our workplace, we abandoned the total contact cast many years ago. This is because many caregivers are not well enough trained to make a good TCC. We have seen many lumpy examples of useless TCCs and have also witnessed several instances where the patient got pressure ulcers from hard edges in a lumpy TCC. If the resources are available, we advise you to use a Walker boot unless you are an expert on making good TCCs.
However, one advantage of a cast is that the patient cannot remove the cast, ensuring better compliance. Many studies have shown that patients do not always adhere to the recommendations and drop the boot within a few weeks of using it when using a removable Walker boot. Patients who are using such a boot will, for example, not be able to drive a car, and this can be enough incentive to take off the boot and store it away in a closet. A work-around solution to this is to apply a few layers of plaster around the boot so that the patient cannot easily remove it.

Figure 15 Walker boots that go high up on the leg reduce the pressure on the sole of the foot by about 40-50%, as long as they fit well. Models which have inflateable air cushions on the inside ensure a very good fit. The patient has to use the boot until the ulcer is completly healed which often means sveral month of use. Understandably this is a burden for many patients and consequently reduces compliance. By applying several rounds of cast around the boot the orthotic can be " locked" so that it cannot be removed but this may not be acceptable for some patients.
Total contact cast (TCC)
A TCC is still seen as the gold standard for offloading diabetic foot ulcers. A TCC that is made correctly will fit the patient's anatomy perfectly, ensuring a good fit. As the name "total contact" implies, the cast should be so well-fitting that it is in total contact with the skin of the leg. As with a walker boot, the cast should be made in such a manner as to allow the patient to ambulate. This often requires some sort of sole to be applied to the base of the cast. One of the advantages of using a cast is that it cannot be removed by the patient ( at least not without considerable effort), increasing compliance. Another advantage of the TCC is that it is relatively cheap and thus one of the most realistic options for many African patients. Remember that it is essential to pad the sole of the foot adequately when using this type of cast. Having self-adhesive wool felt available makes this part a lot easier.
However, an ill-fitting TCC can lead to disaster. We have seen many examples where a poorly made TCC has caused harm to the patient, causing new pressure injuries to the foot. Many diabetic foot patients have sensory neuropathy and will not feel if the cast is causing pressure on parts of the foot! Also, a TCC can give logistical challenges. The patient will have to return regularly to your clinic to remove the cast to change the dressing on the ulcer.
Applying a good TCC is a skill not many caregivers have. In an ideal setting, a specialized cast technician should make this type of cast to avoid complications. Many clinics do not have access to a cast technician. It is, of course, possible to acquire these skills by attending workshops and following step-by-step instructional videos available online. If a Walker boot is simply not a realistic option for your patients because of limited resources, you have no other choice than to become good at making TCCs for these patients.
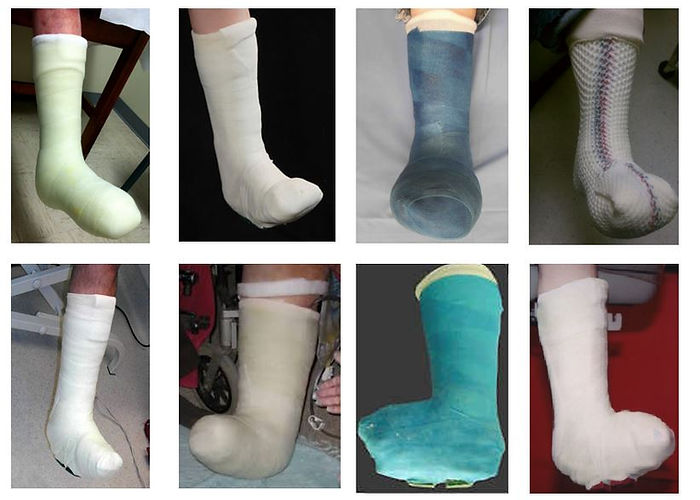
Figure 16 A variety of total-contact casts in various shapes and sizes, and not all of these are well made. An ill-fitting TCC may not provide sufficient offloading and can cause the patient serious harm by making new pressure injuries. A TCC should only be made by someone who has some experience in this type of technique. For this reason a Walker boot is a safer option.

Figure 17 No matter which type of cast material is used, a TCC cannot be used for walking on directly. You always have to use a special type of cast shoe or improvise with some type of rubber sole to allow the patient to weight bear in the cast.

Figure 18 If the patient has the resources to obtain a Walker boot, this is, in our opinion, the best method for offloading the diabetic foot. The image above shows a high Walker boot locked with a few layers of cast material to ensure patient compliance. This type of boot usually fits quite well, is ready-made to walk on, and avoids the common pitfalls of an ill-fitting TCC.
Custom-made total contact cast made of moldable plastic.
Ortothotic companies can deliver custom made contact casts made of a type of plastic material. These are molded on the patients extremity and thus fit perfectly. The patient can usually even choose between different colours and therefore such an orthotic may be more acceptable for some patients. They are usually not as voluminous as a walker boot or a total contact cast. However, as they fit very tight they are not suitable for patients who tend to swell up in their legs during the day. Many patients also complain that they get quite sweaty under this type of orthotic. Furthermore, although they are custom made, they can also cause the patient harm by causing unforeseen pressure to other parts of the foot. Most likely this is an option that is not available to where you work but we simply wanted to show you all the alternatives here.

Figure 19 Custom-made total contact casts made of moldable plastic are usually very expensive and not an option for most African patients.
When the patient doesn't want to do as we advise
Sometimes a patient doesn't want to listen to our advice about offloading. Some patients say it is too cumbersome to go with a lumpy orthotic. The reality, after all, is that the patient, in most cases, will have to use the orthotic or cast for many months. We must take good time to explain to the patient why offloading is the most important aspect of the treatment. Without scaring the patient unnecessarily, we must inform them of the possible consequences if they don't adhere to our advice. Even a tiny diabetes ulcer can lead to amputation if it is not dealt with correctly.
Our goal is to find an offloading solution that is acceptable to the patient. In many cases, we start with self-adhesive wool felt as the first measure while carefully monitoring the effect of this intervention. If the ulcers are not responding to this simple measure within some weeks, most patients will usually understand that more drastic offloading methods will have to be used. Involving the patient's spouse or other family members can also help to ensure compliance.
When the ulcer doesn't respond well despite apparently adequate offloading
Sometimes it seems that we have done everything correctly. The ulcer appears clean, has granulation tissue, and is not smelly, and the patient is using an offloading device, but the ulcer does not want to heal. If you have only been using self-adhesive wool felt at this point, consider using a Walker boot if that is an economical option for the patient. Suppose you are sure that the offloading is adequate and the ulcer will still not heal. In that case, there is usually something wrong with the arterial circulation, or there is undetected osteomyelitis lurking beneath the ulcer. In these cases, always get an x-ray done of the affected foot area. While an x-ray will not catch all cases of osteomyelitis, it will usually be sufficient to rule out severe bone infection. If an MRI is available for the patient, this can be used in cases where a standard x-ray is negative, but there still is a strong clinical suspicion of osteomyelitis.
Even if the wound appears clean, there may still be a bacterial imbalance in the wound that impairs the healing process. This is especially true if there is colonization with Pseudomonas, streptococci, and intestinal bacteria. These strains of bacteria are known to be able to impair healing without necessarily causing an infection. If we have a diabetic foot ulcer that will not heal despite apparently good offloading, we often take a bacterial swab to check who is living in the wound bed. We will obviously always get a positive swab. Usually, there is a mix of different bacteria present, but if the swab shows one or more of the strains mentioned earlier, we should use topical antimicrobials ( not the same thing as antibiotics!) to eliminate these unwanted bacteria. Iodine or silver-based dressings are good examples of what we could apply here.





























